A Common Drug May Make Cancer Immunotherapy Work Better

A newly discovered cancer trick that weakens immunotherapy may be stopped by everyday statins.
Cancer immunotherapy has reshaped modern cancer care by activating the body’s own immune defenses to fight tumors. Drugs known as immune checkpoint inhibitors, which target the PD-1/PD-L1 pathway, have produced long-lasting responses in some patients and created hope for sustained cancer control. However, the majority of patients see only limited benefit. Tumors often adapt and develop ways to avoid detection by the immune system.
Because of this, researchers are now focusing on the biological mechanisms behind immune resistance. Scientists are especially interested in processes that suppress immune activity not just inside the tumor, but throughout the body. One mechanism gaining attention involves small extracellular vesicles (sEVs). These tiny particles released by cancer cells can carry molecules that weaken immune responses, potentially reducing the effectiveness of immunotherapy.
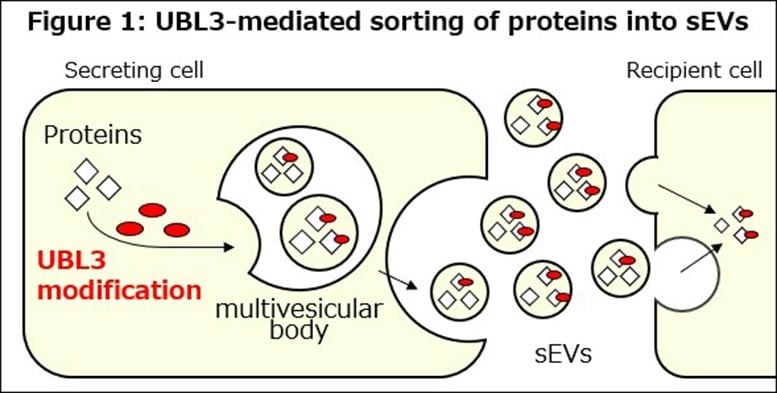
Investigating How PD-L1 Travels in Cancer Cells
To better understand this process, researchers from Fujita Health University in Japan, led by Professor Kunihiro Tsuchida, worked with colleagues, including Dr. Hiroshi Ageta, Dr. Yoshihisa Shimada from Tokyo Medical University Hospital, and Dr. Yusuke Yoshioka and Professor Takahiro Ochiya from Tokyo Medical University. Their goal was to uncover how PD-L1 is selectively packaged into sEVs and whether that process could be targeted with treatment. The study was published in Scientific Reports.
The research centered on a key unanswered question. “Cancer cells release small extracellular vesicles containing PD-L1, which are thought to reduce the effectiveness of cancer immunotherapy. However, how PD-L1 is sorted into these vesicles has remained unclear.” Solving this puzzle became the foundation of their investigation.
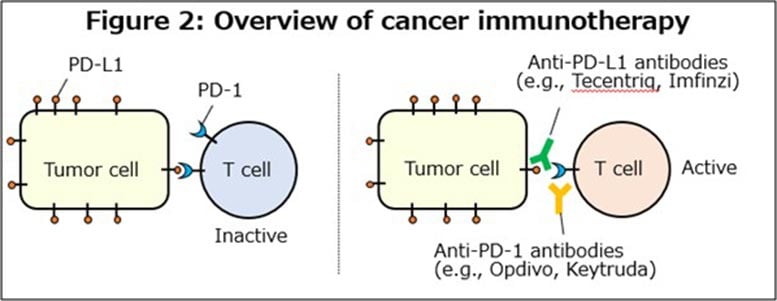
UBL3 Identified as a Key Regulator of PD-L1 Sorting
Using a combination of molecular biology, cell biology, biochemical testing, pharmacological analysis, patient samples, and bioinformatics, the team identified ubiquitin-like 3 (UBL3) as a crucial factor in directing PD-L1 into sEVs.
They discovered that PD-L1 undergoes a previously unknown post-translational modification controlled by UBL3 through the formation of a disulfide bond. This mechanism differs from traditional ubiquitination. Further experiments showed that cysteine 272 within the cytoplasmic region of PD-L1 is the essential site for this modification.
When UBL3 levels were increased, PD-L1 levels inside vesicles rose significantly, even though total PD-L1 within the cells did not change. In contrast, reducing UBL3 expression sharply lowered the amount of PD-L1 packaged into vesicles and released outside the cell. These results confirmed that UBL3 plays a central role in controlling how PD-L1 is sorted into sEVs.
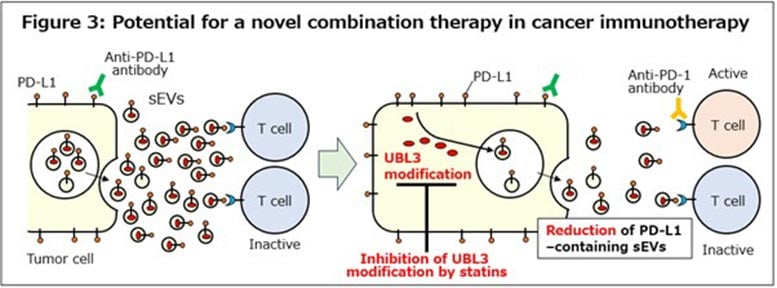
Statins Block the Immune Suppression Pathway
One of the most striking findings was that statins strongly inhibit UBL3 modification. All clinically used statins tested in the study suppressed UBL3 activity, reduced PD-L1 modification, and significantly decreased PD-L1 incorporation into sEVs. These effects occurred at sub-micromolar concentrations that are achievable in clinical settings and were not due to toxic effects on cells.
The researchers also analyzed serum samples from patients with non-small cell lung cancer. Among patients with high tumor PD-L1 expression, those who were taking statins had significantly lower levels of PD-L1-containing sEVs compared with those who were not using statins.
In addition, bioinformatic analysis showed that combined expression levels of UBL3 and PD-L1 were associated with survival outcomes in lung cancer patients. This finding supports the clinical relevance of this regulatory pathway.
A Potential Strategy to Improve Immunotherapy
These findings help explain why immune checkpoint inhibitors fail in many patients. By uncovering a new mechanism that controls the release of immunosuppressive PD-L1 through extracellular vesicles, the study reveals a previously hidden contributor to immune resistance.
The connection to statins is especially significant because these medications are widely prescribed, affordable, and generally safe. This raises the possibility that the discovery could be translated into clinical use relatively quickly. As the researchers noted, “In the long term, this research may lead to more effective and accessible cancer immunotherapies. It could help more patients benefit from immune checkpoint treatments, improving survival and quality of life in real-world settings.”
Opening a New Path to Overcome Immune Resistance
In summary, the study shows that UBL3-driven modification promotes the sorting of PD-L1 into sEVs, while statins can disrupt this process and reduce circulating levels of immunosuppressive PD-L1. By identifying vesicle-associated PD-L1 trafficking as a changeable factor in immune escape, this research points to a new strategy for overcoming resistance to cancer immunotherapy. Adding statins to combination treatment approaches could offer a practical and scalable way to improve outcomes for patients receiving immune checkpoint blockade.
Reference: “Statins attenuate PD-L1 sorting to small extracellular vesicles dependent on ubiquitin-like 3 modification” by Hiroshi Ageta, Yoshihisa Shimada, Tadahiro Nagaoka, Kazuki Takenaka, Yusuke Yoshioka, Kohtaro Konno, Ryosuke Amemiya, Kumiko Nagase, Keisuke Hitachi, Takanori Onouchi, Masahiko Watanabe, Takahiro Ochiya and Kunihiro Tsuchida, 15 December 2025, Scientific Reports.
DOI: 10.1038/s41598-025-27789-x
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
Source link

