Scientists Uncover Dangerous Connection Between Serotonin and Heart Valve Disease
New findings reveal a potential connection between serotonin activity and the progression of a widespread heart valve disorder.
Serotonin is best known for its role in mood, but new research suggests it may also influence how certain heart valve diseases progress. A large multicenter study has found that this common brain chemical could contribute to faster worsening of degenerative mitral regurgitation, a widespread and potentially serious heart condition.
The work, led by researchers at Columbia University in collaboration with the Children’s Hospital of Philadelphia (CHOP), the University of Pennsylvania, and the Valley Hospital Heart Institute, was published in Science Translational Medicine.
When a Heart Valve Stops Sealing Properly
Degenerative mitral regurgitation (DMR) affects the mitral valve, which controls blood flow between the heart’s left atrium and left ventricle. Under normal conditions, the valve shuts tightly with each heartbeat to keep blood moving forward.
In DMR, the valve gradually becomes misshapen and cannot close completely. This allows blood to leak backward toward the lungs, reducing the efficiency of circulation. Over time, the heart compensates by working harder, which can stretch and weaken the muscle.
Early symptoms can be subtle, including fatigue or mild shortness of breath. As the condition advances, it raises the risk of atrial fibrillation, heart failure, and other complications. Millions of people are affected worldwide, particularly older adults, making it one of the most common valve disorders.
There is no medication that can reverse the underlying valve damage. “Certain medications can ease the symptoms and prevent complications, but they do not treat the mitral valve,” says Ferrari, scientific director of the Cardiothoracic Research Program at Columbia. “If the degeneration of the mitral valve becomes severe, surgery to repair or replace the valve is needed.”
A Surprising Link to a Brain Chemical
Serotonin helps regulate mood, sleep, digestion, and blood clotting. It works by binding to receptors on cells, triggering specific responses. Afterward, a protein called the serotonin transporter (SERT or 5-HTT) pulls serotonin back into the cell so it can be reused.
This recycling system is the target of selective serotonin reuptake inhibitors (SSRIs), a widely prescribed class of antidepressants that includes fluoxetine (Prozac) and sertraline (Zoloft). By blocking SERT, these drugs increase the amount of serotonin available in the brain.
What is less widely appreciated is that serotonin signaling also occurs outside the brain, including in heart tissue. Earlier research has linked abnormal serotonin activity to valve thickening in rare drug-related cases, which led scientists to investigate whether a similar mechanism might play a role in common valve diseases like DMR.
What the Data Revealed
The research team analyzed records from more than 9,000 patients who had surgery for DMR and examined 100 mitral valve tissue samples. They found a clear pattern: patients taking SSRIs tended to need surgery at a younger age than those who were not on these medications.
“Studying the data of these patients, we found that taking SSRIs was associated with severe mitral regurgitation that needed to be treated with surgery at a younger age than for patients not taking SSRIs,” says Ferrari.
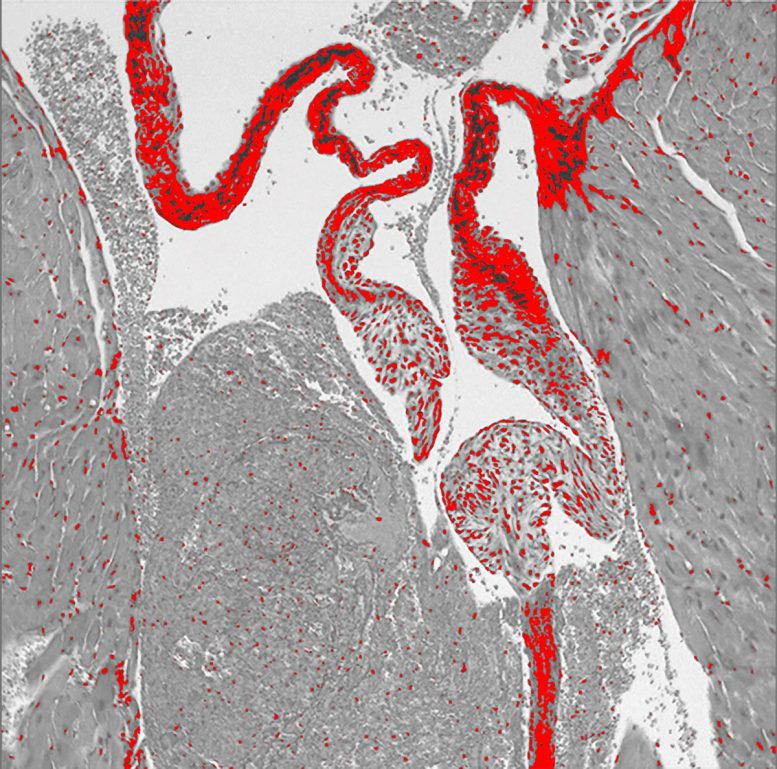
To explore why, the scientists turned to animal models. Mice engineered without the SERT gene developed thicker mitral valves. Normal mice given high doses of SSRIs showed similar changes, suggesting that reduced serotonin reuptake may directly affect valve structure.
The Genetic Piece of the Puzzle
The study also identified a genetic factor that appears to influence risk. Variations in a region known as 5-HTTLPR affect how active the SERT protein is.
People with two copies of the so-called “long” variant have lower SERT activity in mitral valve cells. Among patients with DMR, those with this “long-long” pattern were more likely to require surgery than individuals with other versions of the gene.
At the cellular level, this variant made valve cells more responsive to serotonin, leading them to produce extra collagen. This buildup can stiffen and distort the valve over time. These same cells also reacted more strongly to fluoxetine, indicating that medication and genetics may interact in ways that influence disease progression.
What This Could Mean for Care
The findings point toward a more personalized approach to managing mitral valve disease. A simple genetic test using a blood sample or mouth swab could help identify patients with lower SERT activity who may be at higher risk of rapid progression.
“Assessing patients with DMR for low SERT activity may help identify patients who may need mitral valve surgery earlier,” says Ferrari. “Promptly fixing a mitral valve that is very leaky would protect the heart and could prevent congestive heart failure.”
At the same time, the researchers emphasize that SSRIs remain safe and effective for most people. The study did not find harmful effects in individuals with healthy mitral valves, even when SERT activity was low.
“A healthy mitral valve can probably stand low SERT activity without deforming,” says Ferrari. “It is unlikely that low SERT can cause degeneration of the mitral valve by itself. SSRIs are generally safe for most patients. Once the mitral valve has started to degenerate, it may be more susceptible to serotonin and low SERT.”
Expanding the Serotonin Hypothesis
Follow-up studies suggest that the findings may reflect part of a broader serotonin-related mechanism in valve disease rather than a process limited to degenerative mitral regurgitation alone.
A 2024 study in Cardiovascular Pathology demonstrated that mice lacking the serotonin transporter developed not only thickened mitral valves but also myocardial fibrosis, reduced cardiac function, and age-related remodeling changes across multiple valve structures.
The work also found that mitral valve cells were especially sensitive to serotonin-driven, pro-fibrotic signaling, helping explain why the mitral valve may be particularly vulnerable once degeneration begins.
A second follow-up study, published in 2026 in Frontiers in Cardiovascular Medicine, looked at aortic stenosis, a condition in which the heart’s aortic valve becomes stiff and narrowed. This makes it harder for blood to flow out of the heart to the rest of the body.
The researchers studied patients, mice, and human valve cells grown in the lab. They found that when SERT activity was low and HTR2B signaling was higher, the aortic valve showed more early scarring and calcium buildup. In mice, blocking HTR2B reduced many of these harmful changes, suggesting it could be a possible target for future treatments.
The findings suggest that abnormal serotonin signaling may play a role in more than one type of heart valve disease and could one day help doctors identify higher-risk patients or develop treatments that slow valve damage.
References:
“Decreased serotonin transporter activity in the mitral valve contributes to progression of degenerative mitral regurgitation” by Estibaliz Castillero, Emmett Fitzpatrick, Samuel J. Keeney, Alex M. D’Angelo, Benjamin B. Pressly, Michael T. Simpson, Mangesh Kurade, W. Clinton Erwin, Vivian Moreno, Chiara Camillo, Halley J. Shukla, Vaishali V. Inamdar, Arbi Aghali, Juan B. Grau, Elisa Salvati, Itzhak Nissim, Lubica Rauova, Mark A. Oyama, Stanley J. Stachelek, Chase Brown, Abba M. Krieger, Robert J. Levy and Giovanni Ferrari, 4 January 2023, Science Translational Medicine.
DOI: 10.1126/scitranslmed.adc9606
“Serotonin transporter deficiency in mice results in an increased susceptibility to HTR2B-dependent pro-fibrotic mechanisms in the cardiac valves and left ventricular myocardium” by Estibaliz Castillero, Chiara Camillo, Dov Levine, Alex M. D’Angelo, Yaagnik Kosuri, Juan B. Grau, Robert J. Levy and Giovanni Ferrari, 6 September 2024, Cardiovascular Pathology.
DOI: 10.1016/j.carpath.2024.107689
“Serotonin transporter downregulation is associated with aortic stenosis, and early profibrotic remodeling is mitigated by pharmacological inhibition of HTR2B receptor” by Dov Levine, Chiara Camillo, Estibaliz Castillero, Emre Bektik, Yaagnik Kosuri, Anthony Campbell, Cary Karcher, Abba Krieger, Liming Pei, Ting Peng, Nicole Zeak, Erfan Faridmoayer, Mark A. Oyama, Juan B. Grau, Robert J. Levy and Giovanni Ferrari, 5 January 2026, Frontiers in Cardiovascular Medicine.
DOI: 10.3389/fcvm.2026.1729078
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
Source link

