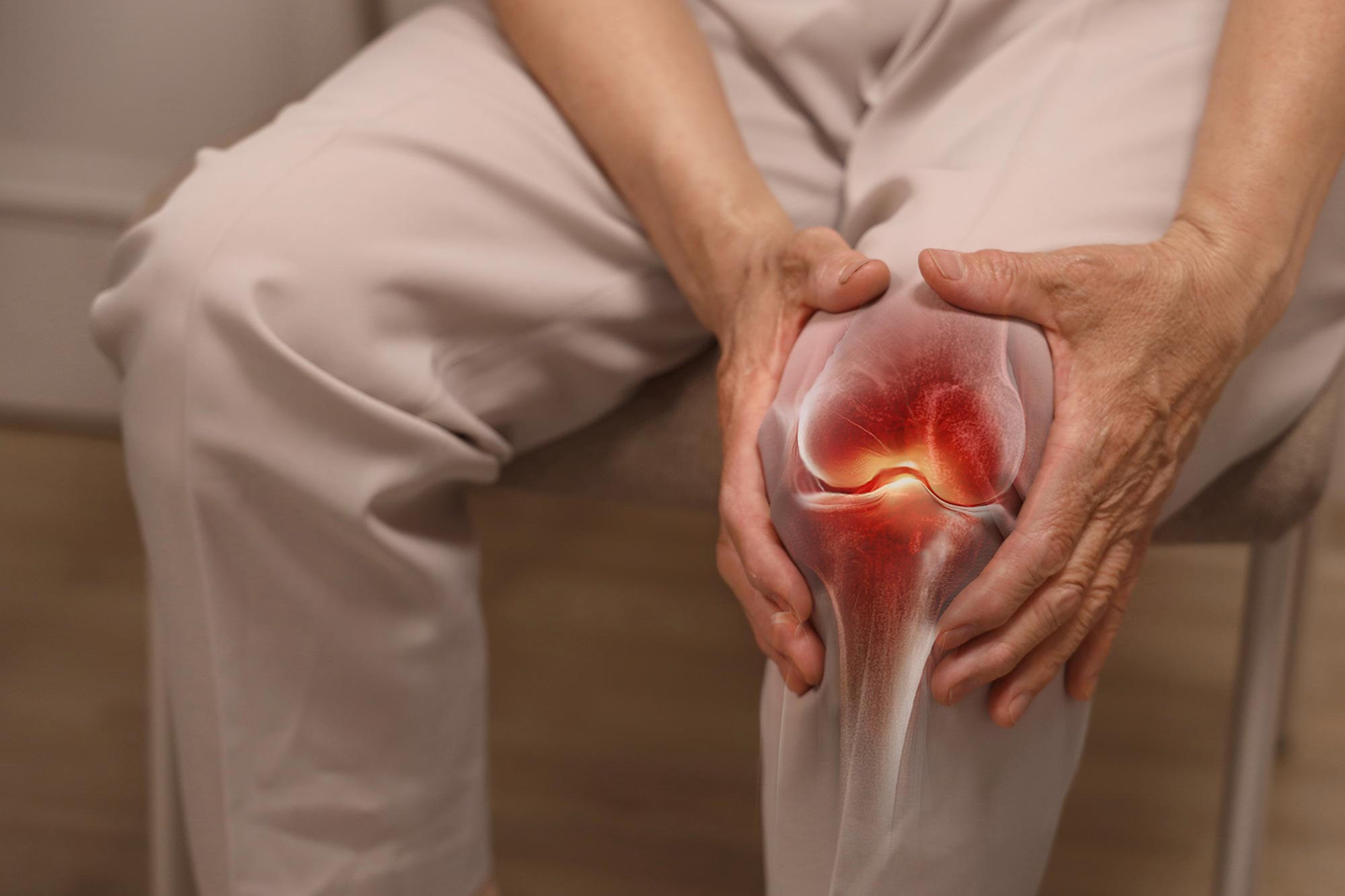
X-rays may do more harm than good in diagnosing knee osteoarthritis, making patients more fearful and more likely to consider unnecessary surgery.
Clinical diagnosis offers a safer, more effective path to managing pain and mobility.
Rising Burden of Osteoarthritis
Osteoarthritis is one of the most common causes of long-term pain and disability, affecting more than two million Australians.
Doctors are generally advised not to rely on routine X-rays to diagnose the condition. Instead, general practitioners can usually confirm osteoarthritis by considering a patient’s symptoms and medical history.
Despite this, nearly half of Australians who first visit their GP with knee osteoarthritis are sent for imaging. These scans cost the health system an estimated A$104.7 million every year.
Our recent research found that using X-rays to diagnose knee osteoarthritis can change how people view their knee pain, and in many cases may lead them to consider knee replacement surgery that might not actually be necessary.
What Happens Inside the Joint?
Osteoarthritis develops when changes inside the joint force it to work harder to repair itself. This process involves the entire joint, including bone, cartilage, ligaments, and muscle.
It occurs most often in older adults, in people with higher body weight, and in those who have previously injured their knees.
For many, knee osteoarthritis brings constant pain and makes simple daily tasks, such as walking or climbing stairs, difficult.
Surgery Isn’t Always the Answer
In 2021–22, more than 53,000 Australians had knee replacement surgery for osteoarthritis.
Hospital services for osteoarthritis, primarily driven by joint replacement surgery, cost $3.7 billion in 2020–21.
While joint replacement surgery is often viewed as inevitable for osteoarthritis, it should only be considered for those with severe symptoms who have already tried appropriate non-surgical treatments. Surgery carries the risk of serious adverse events, such as blood clot or infection, and not everyone makes a full recovery.
Most people with knee osteoarthritis can manage it effectively with:
- education and self-management
- exercise and physical activity
- weight management (if necessary)
- medicines for pain relief (such as paracetamol and non-steroidal anti-inflammatory drugs).
The “Wear and Tear” Myth
A common misconception is that osteoarthritis is caused by “wear and tear.”
However, research shows the extent of structural changes seen in a joint on an X-ray does not reflect the level of pain or disability a person experiences, nor does it predict how symptoms will change.
Some people with minimal joint changes have very bad symptoms, while others with more joint changes have only mild symptoms. This is why routine X-rays aren’t recommended for diagnosing knee osteoarthritis or guiding treatment decisions.
Instead, guidelines recommend a “clinical diagnosis” based on a person’s age (being 45 years or over) and symptoms: experiencing joint pain with activity and, in the morning, having no joint-stiffness or stiffness that lasts less than 30 minutes.
Despite this, many health professionals in Australia continue to use X-rays to diagnose knee osteoarthritis. And many people with osteoarthritis still expect or want them.
Testing X-Rays Against Clinical Diagnosis
Our study aimed to find out if using X-rays to diagnose knee osteoarthritis affects a person’s beliefs about osteoarthritis management, compared to getting a clinical diagnosis without X-rays.
We recruited 617 people from across Australia and randomly assigned them to watch one of three videos. Each video showed a hypothetical consultation with a general practitioner about knee pain.
One group received a clinical diagnosis of knee osteoarthritis based on age and symptoms, without being sent for an X-ray.
The other two groups had X-rays to determine their diagnosis (the doctor showed one group their X-ray images and not the other).
After watching their assigned video, participants completed a survey about their beliefs about osteoarthritis management.
How Imaging Shapes Beliefs
People who received an X-ray-based diagnosis and were shown their X-ray images had a 36% higher perceived need for knee replacement surgery than those who received a clinical diagnosis (without X-ray).
They also believed exercise and physical activity could be more harmful to their joint, were more worried about their condition worsening, and were more fearful of movement.
Interestingly, people were slightly more satisfied with an X-ray-based diagnosis than a clinical diagnosis.
This may reflect the common misconception that osteoarthritis is caused by “wear and tear” and an assumption that the “damage” inside the joint needs to be seen to guide treatment.
Rethinking Osteoarthritis Care
Our findings show why it’s important to avoid unnecessary X-rays when diagnosing knee osteoarthritis.
While changing clinical practice can be challenging, reducing unnecessary X-rays could help ease patient anxiety, prevent unnecessary concern about joint damage, and reduce demand for costly and potentially unnecessary joint replacement surgery.
It could also help reduce exposure to medical radiation and lower health-care costs.
Previous research in osteoarthritis, as well as back and shoulder pain, similarly shows that when health professionals focus on joint “wear and tear” it can make patients more anxious about their condition and concerned about damaging their joints.
If you have knee osteoarthritis, know that routine X-rays aren’t needed for diagnosis or to determine the best treatment for you. Getting an X-ray can make you more concerned and more open to surgery. But there is a range of less-invasive non-surgical options that could reduce pain and improve mobility.
Written by
- Belinda Lawford – Senior Research Fellow in Physiotherapy, The University of Melbourne
- Kim Bennell – Professor of Physiotherapy, The University of Melbourne
- Rana Hinman – Professor in Physiotherapy, The University of Melbourne
- Travis Haber – Postdoctoral Research Fellow in Physiotherapy, The University of Melbourne
Adapted from an article originally published in The Conversation.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Source link